Two Decades of Lyme Disease: What’s Next?
Can twenty years completely transform how we understand something once wrapped in confusion and doubt? Absolutely. What began as a tick-borne illness that left families and clinicians frustrated has evolved into a story of progress, persistence, and growing clarity. Have breakthroughs sparked real hope? Yes, they have. Do lingering myths and inconsistent approaches still leave people searching for answers? Without question. So where does it stand today after all this time? It stands stronger, more recognized, and more openly discussed than ever before—yet still pushing us to ask sharper questions, demand better solutions, and refuse to settle for uncertainty.
Here comes a closer look at past developments, scientific advances, present insight, along with what may arrive next for this condition after two decades.
Basics: What Is Lyme Disease?
It’s an illness triggered by bacterium Borrelia burgdorferi and spreads to people through bites from infected black-legged insects, often called deer types. It tends to show up most in the northeastern, north-central, and some Pacific regions of the U.S., though cases have popped up nationwide.
Typical early symptoms include:
Fever
Fatigue
Headache
Muscle and joint aches
A distinctive “bull’s-eye” skin rash called erythema migrans
Without timely treatment, it can move beyond an initial site and travel deeper into a person’s system. Over time, inflammation may develop within joints, leading to stiffness or persistent discomfort. Cardiac involvement may follow, sometimes affecting rhythm or overall function. Nervous pathways may also become involved, resulting in changes related to sensation, focus, or coordination.
A Look Back: Lyme Disease in the Early 2000s
In the early 2000s, this illness finally started gaining wider public attention—but did that mean clarity followed? Not at all. Many people still searched for straight answers and found only confusion. Were tests reliable back then? Often, no. Without a classic skin marker, countless individuals were misidentified, overlooked, or even told their struggles were imagined. Can you imagine being dismissed while knowing something wasn’t right? That frustration was real—and for many, it marked the beginning of a long, exhausting fight to be believed.
Medical professionals often failed to agree. Some followed official recommendations closely, relying on a short course of antibiotics as a standard approach. Others believed lingering symptoms reflected an ongoing problem and argued for longer treatment. This divide fueled intense debate and, at times, even legal action against those who chose paths outside accepted norms.
Back then, many patients lived in limbo, battling disabling symptoms with few answers.
Diagnostic Advances: Better, But Not Perfect
Twenty years later, testing methods show modest improvement. A two-step blood test recommended by CDC still stands as a primary option. It involves:
ELISA test to detect antibodies.
A follow-up test, often called a Western blot, was used to check for certain antibodies tied to the infection.
Still, these tests remain imperfect. False negatives can appear, particularly during early stages when a person hasn’t produced sufficient antibodies. In long-standing cases, results may turn unclear or inconclusive, leaving uncertainty even after testing.
In 2019, FDA cleared updated versions of a two-step testing approach that aim to improve accuracy along with speed, yet no option works as a guaranteed solution. Some laboratories promote non-standard testing methods, which remain controversial and lack broad acceptance within mainstream practice.
Chronic Lyme Disease vs. Post-Treatment Lyme Disease Syndrome (PTLDS)
For two decades, one question has refused to fade: when lingering symptoms remain after an initial infection, does that mean something deeper is still unfolding—or was it only meant to be brief? Are those ongoing struggles simply echoes of the past, or signs that the battle never truly ended? Many have asked, many have doubted, and many have lived the uncertainty. Yet one truth stands firm—persistent challenges are real, they matter, and they deserve answers that go beyond dismissal or delay.
Many patients continue to suffer long after treatment—experiencing fatigue, joint pain, brain fog, and more. This has led to the term Post-Treatment Lyme Disease Syndrome (PTLDS), recognized by CDC and other major health bodies.
Here lies a key complication: PTLDS does not automatically suggest bacteria remains active. It may involve:
A lingering immune response that continues reacting long after an initial trigger fades.
Permanent tissue damage.
Another overlapping condition.
At the same time, clinicians with deeper experience argue that a lingering organism may still be present and that longer medication plans could bring meaningful relief. Could something remain hidden beneath the surface? Could extended care make a real difference? Many believe so—and they’ve seen lives improve because of it. While a gap still separates mainstream views from alternative paths, one truth is gaining ground: ongoing struggles are real, they run deep, and they can reshape everyday life in powerful, lasting ways.
Tick Numbers Increasing: An Expanding Public Concern
Shifts in climate patterns, forest restoration efforts, along with expanding suburban development have each played a role in boosting numbers while extending reach. As a result, these insects now appear across wider regions and remain active across longer stretches of each year.
Reports indicate case counts within U.S. more than doubled across last twenty years. Several estimates suggest over 476,000 individuals receive diagnosis and treatment each year.
Still, many experts believe real numbers climb far higher, since countless cases never make it into official reports. How many people are quietly struggling without being counted? How many stories go unheard simply because they were never recorded? That invisible gap transforms this from a clinical issue into a nationwide concern—one that reaches beyond exam rooms and into communities, workplaces, and homes across America.
Evolving Treatments: What’s Changed?
Standard care still leans on a focused course of antibiotics—most often doxycycline, amoxicillin, or cefuroxime. Does this approach work for many people? Yes, especially when started early. Is it always enough for everyone? Not always—and that’s where conversations grow deeper. For countless individuals, these medications mark the first powerful step toward reclaiming strength and stability.
During early stages, response often proves strong. Yet later stages or PTLDS situations tend to bring slower or incomplete recovery.
Alongside this, various experimental or integrative options gained attention, including:
Herbal protocols like the Buhner or Cowden protocols
These options aren’t officially approved for this illness, yet many turn to them when conventional methods fall short. Why would someone explore alternatives? Because when progress stalls, hope pushes people to look beyond the usual path. And do some find real relief through a more personalized, whole-person approach? Yes—countless individuals say tailoring strategies to their unique needs has brought renewed strength, clarity, and a sense of control they thought was lost.

A New Perspective: Ways This Condition Influences Thinking and Emotion
Awareness keeps expanding around emotional changes linked to this illness. Can it affect mood and thinking in powerful ways? Yes, it can. Many have faced waves of depression, anxiety, sudden panic, and even episodes that feel frightening or unfamiliar—all connected to infection. Is it “just stress,” or something deeper happening beneath the surface? For many, it’s far more than stress, and recognizing that truth has opened the door to more honest conversations and real validation.
Recent findings suggest that Borrelia may disrupt central nervous pathways, setting off neuropsychiatric changes that closely resemble other illnesses. Could an infection really mimic entirely different diagnoses? Surprisingly, yes. It can present in ways that look like attention disorders, mood instability, or even memory decline—blurring lines and complicating answers. That possibility challenges assumptions and reminds us to look deeper when patterns don’t quite add up.
Bipolar disorder
Alzheimer’s disease
Multiple sclerosis
Unfortunately, this often leads to misdiagnosis and mistreatment. Patients are sent to psychiatrists instead of infectious disease specialists, prolonging their struggle.
Across twenty years, this mind–system connection gained wider acceptance, even as further research remains necessary.
Special Considerations for Children
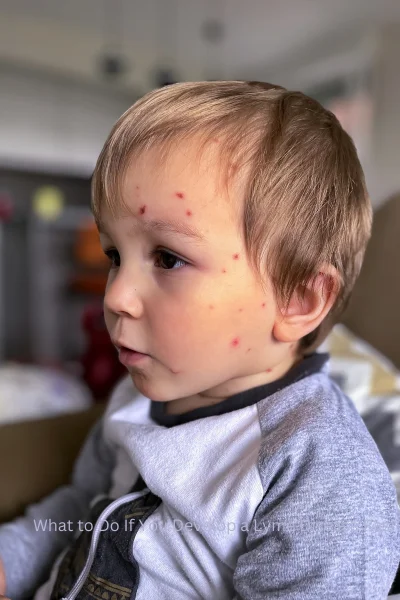
Children carry greater vulnerability, spending long hours outdoors while natural defenses are still developing. Does that increase exposure risk? Absolutely. And have reported cases in this age group risen sharply over the past two decades? Yes, they have—and that rise demands attention. When active, curious kids suddenly seem different, parents notice. That shift isn’t imagined, and it shouldn’t be overlooked.
Symptoms in children can include:
Mood swings
Academic regression
Behavioral changes
Joint pain or fatigue
Parents frequently describe noticing a “different child” after infection. Delays around recognition and treatment occur often, and lasting effects on thinking patterns along with emotional development can feel deep and far-reaching.
Growing Advocacy and Expanding Awareness
One major shift across recent years involves a surge in patient advocacy. Social platforms, documentary projects such as Under Our Skin, along with well-known voices sharing personal journeys pushed this issue into public view.
When public figures like Avril Lavigne, Shania Twain, and Justin Bieber spoke openly about their personal struggles with this illness, did it change the conversation? Absolutely. Their honesty shattered silence, eased stigma, and made millions pay attention. When global stars admit they’ve faced exhaustion, uncertainty, and long recoveries, it sends a powerful message: this is real, it can affect anyone, and it deserves serious funding and national focus.
Grassroots groups also stepped forward, playing a crucial role in:
Pushing for better testing
Lobbying for insurance coverage
Supporting patients emotionally and financially
Back in early 2000s, people facing it often felt ignored or unheard. Today, they carry a far stronger voice along with broader community connections that amplify experiences and push conversations forward.
Research Breakthroughs: A Glimmer Ahead
Over the past two decades, funding dedicated to this illness has grown significantly, opening doors to promising new directions. Has that investment made a difference? Absolutely—it has accelerated innovation, expanded scientific exploration, and sparked fresh momentum. Are breakthroughs finally within reach? Many believe so. Increased financial commitment has fueled advanced drug development, vaccine exploration, and deeper biological mapping—bringing renewed optimism that stronger answers are not just possible, but closer than ever.
- Development of newer antibiotics that may remove bacteria more efficiently
Vaccine candidates under investigation, including work from Pfizer along with Valneva
Biofilm-focused studies revealing how Borrelia shields itself from immune response
Genomic sequencing efforts designed to map strain differences and behavior patterns - Ongoing scientific efforts are also exploring potential links between this illness and autoimmune disorders like lupus or rheumatoid arthritis. Could an infection trigger immune confusion that lingers long after the initial exposure? Many experts believe it’s possible. And if those connections are confirmed, would that reshape how long-term complications are understood? Absolutely—it could transform both diagnosis and long-range management, offering clearer answers to people who have searched for them for far too long.
Even with encouraging advances, does progress feel fast enough when weighed against real-world impact? Not quite. Why does momentum still seem slower than it should be? Because funding continues to trail behind many other infectious illnesses, narrowing both speed and scope of discovery. Can breakthroughs happen without strong financial backing? Rarely. Greater investment fuels innovation, accelerates answers, and shortens the wait for meaningful change—something millions are still hoping to see.
Global Impact: Not Just a U.S. Problem
Although this illness is often associated with the United States, is it confined to one nation? Not at all. It has surfaced across continents, crossing borders and climates alike. From North America to Europe and parts of Asia and Australia, documented cases continue to emerge. Does that global reach change the conversation? Absolutely—it reminds us this is not a regional issue but an international challenge that calls for worldwide awareness and coordinated action.
Canada
Europe
Russia
China
Australia
In fact, European strains of Borrelia differ slightly, leading to varied symptoms. For instance, neurological symptoms may be more prominent in European cases, while Americans tend to experience more joint-related issues.
As international travel and climate change continue to influence disease spread, global coordination will be crucial.
Living Through It: Stories from Survivors
Ask anyone who’s battled this illness for years, and what will they tell you? They’ll speak about misdiagnoses that led them down the wrong path, about doctor after doctor offering shrugs instead of answers, about savings drained while searching for relief. Was it exhausting? Absolutely. Was it discouraging? More than words can capture. Yet will they also tell you something powerful? Yes—they’ll talk about resilience, about refusing to give up, about turning frustration into fierce determination. Their stories aren’t just about struggle; they’re about strength rising in the face of uncertainty.
Misdiagnoses (everything from lupus to fibromyalgia to MS)
Doctor after doctor shrugging their shoulders
Spending tens of thousands on treatment
But you’ll also hear resilience.
Patients have learned to advocate for themselves, navigate broken systems, and build supportive communities. Many turn their pain into purpose, becoming coaches, advocates, or nonprofit leaders.
These stories are not just about disease. They’re about human strength and the pursuit of truth.
Looking Ahead: Changes Needed Over Next Twenty Years
If one lesson stands out after two decades, it’s this: this isn’t just a simple insect bite. Is it deeper than that? Without question. It carries layers of medical uncertainty, emotional weight, and even political friction that have shaped countless lives. Can future decades look different? They must. But that will only happen if real shifts occur—clearer diagnostics, more flexible care strategies, stronger funding, broader physician education, and greater public awareness. Progress is possible, but only if bold changes move from conversation into action.
Better diagnostics—especially in early infection.
Should medical guidance follow a rigid script when every person’s experience is different? Of course not. More flexible medication guidelines that recognize individual variability are essential. Can one approach truly fit everyone? Rarely. When care plans adapt to unique responses, history, and severity, outcomes improve—and people feel seen rather than sidelined. Flexibility isn’t weakness; it’s smart, patient-centered progress.
More research funding, especially into long-term illness.
Insurance reforms to cover longer or experimental treatments.
Should clinicians rely only on textbook cases when real-life presentations rarely follow a script? Of course not. Stronger education is essential so medical professionals can recognize subtle, non-classic patterns that don’t fit the usual mold. Could earlier recognition change outcomes? Absolutely. When providers are trained to look beyond obvious signs, fewer people are dismissed, fewer cases are missed, and more lives move toward clarity instead of confusion.
Public awareness so people protect themselves—and know what to do after a tick bite.
Final Thoughts: A Journey of Understanding and Healing
Two decades ago, it was widely misunderstood and often dismissed. Has that changed? Yes—though complexity still remains. Are we further along than before? Absolutely. Meaningful progress is visible, conversations are louder, and advocacy is stronger than ever. With deeper scientific commitment, fearless voices demanding accountability, and a renewed focus on compassion, could the next era finally bring clear answers and lasting relief? Many believe it can—and momentum is building in that direction.
Whether newly diagnosed or facing symptoms for years, remember this: you are not alone, and this fight continues.
FAQs
Can long-term effects be managed?
Yes, while managing long-term effects can be challenging, there are various approaches that help minimize their impact. Many people manage symptoms through physical therapy, diet modifications, and medications targeted at specific symptoms like pain, fatigue, and joint stiffness. Regular exercise, maintaining a healthy lifestyle, and engaging in stress-relieving practices such as meditation can also improve overall well-being and support long-term recovery. Consulting with specialists, such as rheumatologists or neurologists, may be necessary to address specific concerns.
How does this condition impact daily activities?
For many, daily routines become limited by ongoing pain, deep fatigue, along with thinking challenges. Simple actions such as walking, working, or managing a household may grow harder over time. Quality of life often declines, pushing people toward changes like cutting back on workload or relying on others for certain tasks. Recognizing how it affects personal functioning and adjusting routines at home along with work settings can ease day-to-day strain.
What are some lifestyle changes that can help manage symptoms?
Can daily habits truly influence how someone feels while navigating this illness? Absolutely. Small, intentional shifts—like building in more rest, lowering stress, and choosing gentle, low-impact movement—often make a noticeable difference. Does food matter? Yes, focusing on anti-inflammatory choices can ease joint and muscle discomfort. And what about calming the mind? Practices such as yoga, deep breathing, and meditation can steady emotions and restore balance. These changes may seem simple, but together they create a powerful foundation for greater strength, clarity, and resilience.
How do environmental factors contribute to symptoms?
Environmental factors, such as changes in weather or exposure to allergens, can exacerbate symptoms for some individuals. For instance, cold, damp weather might increase joint pain, while high-stress environments or poor air quality could worsen cognitive issues or fatigue. Being mindful of these environmental triggers and making adjustments, like using humidifiers, dressing warmly, or taking breaks from stressful situations, can make a significant difference in symptom management.
What support systems are available for people dealing with this illness?
Can anyone navigate a long, exhausting journey alone? Rarely. Reliable networks make a powerful difference when challenges refuse to fade. Do people feel stronger when they connect with others who truly understand? Absolutely—peer communities, whether in person or online, bring reassurance and real-world insight that can’t be found in silence. Can experienced practitioners guide long-term management with thoughtful strategies? Yes, and that direction often restores confidence. And what about emotional strain that builds over time? Honest conversations with trained professionals can lighten that weight, steady the mind, and remind someone they don’t have to carry it all by themselves.
Are there any new therapies or treatments being developed?
Is progress still moving forward? Absolutely. Scientists continue exploring better medication options, especially for those facing long-lasting effects. Are new approaches showing promise? Yes—advances in immunotherapy, targeted anti-inflammatory drugs, and neuroprotective strategies are opening hopeful possibilities. What about complementary paths? Acupuncture, herbal supplements, and specialized nutrition plans are also being examined for their potential to ease lingering challenges. And are clinical trials still underway? Without question. Staying informed and having open conversations with a trusted medical professional can keep you aware of emerging options and empower you to make confident decisions about what comes next.



