How can a little one stay engaged while building strength and coordination? Gentle conversation, playful interaction, and frequent encouragement can make a big difference. Why include an affected side during play? Because small, playful movements often spark awareness and gradual improvement. Simple games, cheerful songs, or reaching activities can inspire motion and curiosity. What about tiny actions like touching toys, clapping hands, or grasping objects? Those moments quietly build strength and coordination over time. When play feels joyful and interactive, connection grows stronger, creating a warm, positive space where steady progress and improved motion can unfold little by little.
Newborns’ Brachial Plexus Injury: Parent Guide
Picture a joyful second—baby arrives, hearts bursting with happiness—yet a quiet worry appears when one tiny arm hangs limp. Could a nerve concern be limiting movement through shoulder, arm, or hand? Many families ask that same question. During a challenging birth, especially with a bigger newborn, pressure around delicate nerves can occur. Is such a moment common? Not really—roughly one to three in a thousand births—but families across America have walked this path and seen progress. A visit with a doctor brings clarity and steady guidance, and soon strength can grow as little one begins reaching, gripping, and moving forward with bright confidence.
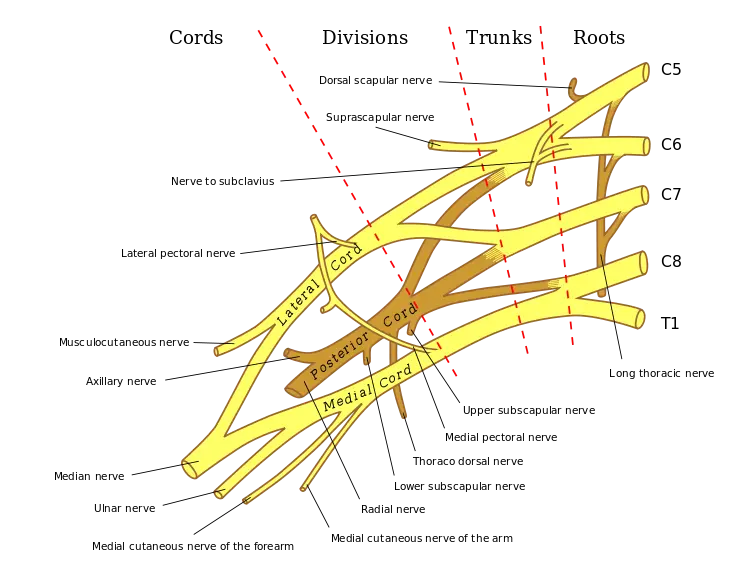
There are four main types of injuries in newborns:
| Type of Injury | Description |
| Neuropraxia | Mildest form; temporary conduction block due to myelin sheath damage |
| Axonotmesis | More severe; nerve fibers disrupted but myelin sheath intact |
| Neurotmesis | Most severe form, involving complete disconnect that requires rebuilding function entirely from scratch. |
| Erb’s Palsy (C5-C6) | Upper plexus injury; affects shoulder and elbow flexion |
| Klumpke’s Palsy (C8-T1) | Lower plexus injury; affects wrist and hand function |
| Total Plexus Palsy (C5-T1) | All nerves involved, resulting in total paralysis of arm |
Could a tiny stretch along a fragile nerve pathway really pause motion or feeling for a while? Yes, and that situation is known as neurapraxia, a very common nerve injury where fibers stretch but stay intact. Does such a moment sound frightening at first? Of course—but good news often follows. In many newborn cases, movement or sensation fades briefly yet slowly returns as natural repair begins working quietly inside. Does recovery truly happen? In most situations, absolutely—strength and normal activity often come back within several weeks or a few months, bringing renewed comfort and confidence as gentle nerve signals start flowing again.
What happens when a nerve pathway breaks completely and signals can no longer travel forward? That severe condition is known as neurotmesis. In this situation, nerve fibers become fully torn, stopping communication between muscles and brain. Sounds alarming, right? Sadly, recovery at this stage often becomes far more challenging. Progress may arrive slowly, and improvement sometimes remains limited. Even with consistent rehabilitation approaches, full restoration does not always occur, leaving only partial return of strength or movement in certain cases.
Avulsion represents an even more severe condition, marked by full separation of nerve roots from spinal region. Once this type of injury occurs, return of normal motion is highly uncommon, as signal transmission pathways have been completely disrupted.
Could a delicate nerve route near spinal area face strain during breech birth? Yes, such a situation can involve a lower portion of that network. What might appear afterward? In some newborns, weakness shows up along one lower limb, and movement may look limited or uneven. Does coordination sometimes look off on that side? It can, with balance appearing slightly reduced for a while. Still, careful observation and gradual progress often bring encouraging changes as strength and control slowly return over time.
| Type of Injury | Prognosis |
| Neuropraxia | Most recover fully within 3 months |
| Axonotmesis | Often recovers within months, but may not be complete |
| Neurotmesis | Recovery possible, but often requires surgery and extensive therapy |
| Erb’s Palsy (C5-C6) | Good prognosis, often recovers within 6 months |
| Klumpke’s Palsy (C8-T1) | More challenging prognosis, may require long-term therapy |
| Total Plexus Palsy (C5-T1) | Variable prognosis, depends on severity and treatment |
Main cause in infants often involves excessive pulling or twisting near neck area during delivery. Chances increase when newborn is larger in size, maternal pelvis is narrow, or birthing process becomes prolonged or complicated.
Additional potential causes:
Shoulder dystocia:
This occurs when a baby’s shoulder becomes stuck behind a parent’s pelvic bone during birth.
Why might a medical team bring out forceps during childbirth? Sometimes extra guidance becomes necessary when progress slows. Metal instruments gently cradle an infant’s head and guide passage outward with precision. When skilled hands guide placement, birth often becomes easier, even in challenging moments. But what if pressure grows too strong or alignment shifts slightly? Nearby nerves and soft tissue can experience strain. What might appear afterward? A newborn may show reduced sensation or limited motion along an upper limb. Is recovery possible? In many mild situations, motion gradually returns with time as nerve activity settles. In more severe cases, improvement may take longer, and arm movement can remain partly restricted depending on how much pressure occurred during delivery.
Why might a medical team choose vacuum extraction near final moments of childbirth? Sometimes extra guidance becomes necessary as an infant moves through a birth canal. A soft suction cup rests gently on an infant’s head, creating light traction that encourages forward movement. When placement is accurate and handled with steady skill, delivery often becomes easier and more controlled. But what happens if alignment shifts or pressure grows too strong? Delicate nerves and soft tissue can face strain. What might appear afterward? A newborn could show difficulty with motion or coordination soon after birth. Does recovery still occur? In many mild situations, movement gradually improves as nerve activity stabilizes. In more severe situations, challenges with motion or muscle control may remain for a longer period, depending on how much pressure occurred during delivery.
What happens when a little one faces NBPP? Worry often rises, yet many families have walked a similar road and found steady progress ahead. Guidance and clear information remain available through experienced professionals and community programs focused on improving movement and strength. Could a specialist point parents toward skilled rehabilitation teams? Absolutely—trained therapists often design personalized exercises that encourage gradual improvement. Does patience truly make a difference? Yes, steady attention and encouragement frequently lead to meaningful gains, allowing many children to regain movement step by step while confidence grows stronger with time.
In the interim, there are several proactive measures you can take to aid your baby dealing with NBPP:
- Cultivate patience and surround that little one with plenty of love, as recovery for most NBPP cases unfolds gradually through steady progress over time.
- Learn gentle positioning techniques for a little one to maintain flexibility and prevent stiffness or joint restriction.
- Consider gentle movement with little one—could simple stretches and playful motions keep joints flexible while muscles grow stronger? Absolutely. Slow, careful activity encourages natural movement through shoulder, arm, and hand, allowing strength to build step by step while bonding moments grow sweeter. With patience and consistency, progress often becomes visible as tiny fingers reach, grasp, and explore world with growing confidence.
Could connecting with folks facing similar hurdles ease a tough journey? Absolutely. A group focused on NBPP offers shared stories, encouragement, and reassurance, reminding families that progress and hope remain possible.
Always keep this close to heart—little one carries grit and quiet toughness. Wondering if bright days still lie ahead despite NBPP? Absolutely. With steady love and strong encouragement from a caring parent, a child often finds strength to push forward, learn new movements, and grow with remarkable determination. Step by step, confidence can rise, proving that courage and patience open a path toward a hopeful future.

When a little one faces difficulty soon after birth, a parent might sense something unusual right away—or signs may appear gradually with time. Why does that happen? Because each situation differs depending on which nerves or movements face disruption and how deep that challenge runs. Some infants show clear signs early, while in many cases changes become noticeable only as weeks pass. Understanding this possibility brings clarity and encourages close observation as a child continues growing and developing.
Look out for these common signs:
- Lack of strength or movement in that side or hand.
- Reduced motion or sensation on that side.
- That side showing limited motion may appear slightly different or rest in an unusual position.
- Difficulty moving fingers or thumb
- What if a Moro reflex shows on only one side? This reflex usually makes a little one spread limbs wide and pull them back in. When only one arm moves, it may signal reduced strength or motion on the opposite side.
Doctors often identify this condition in a newborn through a detailed physical check and review of medical history. In some cases, additional imaging such as X-rays, ultrasounds, or MRIs may be recommended to confirm details and determine extent of nerve involvement.
| Symptom | Description |
| Limited movement or strength on one side. | How can muscle performance change when nerve signals become disrupted? It often depends on severity and location along a nerve pathway. Common signs may include: |
| * Erb’s palsy: Arm hangs limp, inability to raise arm above shoulder, weak grip. | |
| * Klumpke’s palsy: Claw hand, weak wrist and finger flexion. | |
| Total brachial plexus condition: complete loss of motion and sensation across an entire upper limb. | |
| Reduced motion or sensitivity in an upper limb | This may vary from slight tingling to total loss of feeling, depending on which nerves are involved. |
| Unusual Placement of That Side | That side showing limited movement may stay fixed in one position, often with elbow bent and arm held close, or it might hang loosely without much control or response. |
| Missing Moro reflex on affected side | Moro reflex acts as a natural startle response where a little one spreads arms wide. When this reaction appears on only one side, it can suggest an issue affecting that particular area. |
| Decreased grip strength on an affected side. | An infant may show a weak grasp or be unable to hold objects altogether. |
| Pain (less common in newborns) | Though uncommon in newborns, some may experience discomfort on that side or near shoulder region. |
Long-Term Challenges a Kid Might Face After This Kind of Setback
| Challenge | Description |
| Upper Limb Weakness | Difficulty using that side because muscles lack normal strength. |
| Pain and Spasticity | Ongoing soreness and tight muscles in that side can make everyday movement tough. |
| Sensory Loss | Less or no feeling in that side. |
| Joint Deformities | Tightness or joint shifts may occur in that area, making movement increasingly difficult over time. |
| Psychological Impact | Emotional ups and downs, along with social challenges that arise after an experience like this, can place a heavy strain on an individual. |
When something feels off with a little one’s movement, what happens next depends on how serious things are and which areas are involved. In many cases, gentle motion exercises and everyday skill practice become part of recovery. One method focuses on improving coordination and flexibility through guided activity, while another teaches families to include that side naturally during feeding, dressing, or playtime. Combining both methods encourages steady progress, allowing a child to grow more confident and capable as strength and motion gradually return.
For less severe cases, non-surgical approaches take precedence, encompassing:
Physical Therapy: A physical therapist guides parents in gentle movement exercises for an infant’s affected arm and hand, reducing stiffness and contractures while encouraging steady flexibility and comfort.
Occupational Therapy: Occupational therapists guide families in including an affected limb during daily routines like eating and dressing, encouraging natural use and improved coordination over time.
Splinting or Casting: Use of splints or casts maintains affected arm in a position that promotes proper healing and reduces strain throughout recovery.
Medication: Use of prescribed medication to ease any discomfort an infant might experience during recovery.
In more serious situations, surgery may become an option, often considered when a child reaches about three to six months of age. Why wait until that stage? Specialists usually evaluate early progress first before deciding if a procedure could make a difference. When needed, surgery may focus on repairing injured nerves or transferring muscles from one area to improve movement and strength. Goal centers on improving overall function and creating a stronger path toward recovery, giving a little one a better chance to move, play, and grow with greater ease and confidence.
| Treatment | Advantages |
| Non-operative Management | – Minimally invasive – Allows natural recovery to occur over time. – Lower risk of complications |
| Nerve Grafting | – Improves functional outcomes for severe injuries – Can restore sensation and function |
| Neurolysis | Easing pressure around an affected area allows nerve signals to flow again. As strain fades, function often improves gradually, bringing slow return of motion and sensation over time. – Can restore movement and sensation more effectively. |
| Muscle Transfers | – Provides alternative function for paralyzed muscles – Improves quality of life |
After an operation, a little one often needs gentle guidance to start moving that side again and gradually build strength. Wondering how long progress might take? A few months in many cases—sometimes a bit longer. Patience during this stage truly matters. With steady encouragement, loving attention, and consistent guidance, most kiddos regain movement step by step, growing stronger and more confident as weeks pass. Before long, many return to playful, active childhood filled with laughter and bright moments.
What lies ahead for a little one in this situation? That often depends on how much was affected and exactly where. In many cases, children gradually regain movement and grow stronger as months pass—so hopeful progress is absolutely possible. Still, some may continue facing challenges with motion or strength on one side. Each journey unfolds a bit differently, yet patience, encouragement, and attentive guidance can make a meaningful difference as a child keeps growing and discovering new abilities along the way.
Financial Assistance and Insurance Guidance
Raising a little one facing this kind of challenge calls for patience, strength, and a whole lot of heart. Do long or uncertain days sometimes feel overwhelming? Of course—but steady love from a caring parent often becomes a child’s strongest anchor. Quiet reassurance and small moments of encouragement can carry incredible power. Step by step, hope and determination can open a path toward steady progress. Here are a few simple, down-to-earth tips to guide a devoted parent along this meaningful journey.
Hang in there—healing from this type of nerve damage takes time. Stay positive, and don’t get discouraged if progress isn’t immediate.
Find a circle that understands—can shared stories lift heavy moments along this journey? Absolutely. When we connect with parents and families walking similar paths, comfort grows in ways words can hardly capture. Honest stories, practical ideas, and warm encouragement spark fresh strength on hard days. With patience, compassion, and good people around us, a parent and little one move past challenges, celebrate each small victory, and keep finding joy in simple moments.
Acknowledge every bit of progress, no matter how small—could tiny steps forward still mean something big? Absolutely. Noticing each improvement and celebrating those moments sparks motivation and builds confidence in a child. That steady recognition of effort encourages persistence and strengthens determination. Over time, a positive mindset grows, turning each small step into a meaningful milestone worth celebrating.
Find a circle that understands—could shared experiences lighten heavy moments along this journey? Absolutely. Connecting with parents and families who faced similar paths brings comfort words can hardly express. Stories, advice, and simple encouragement often spark renewed strength during difficult days. With patience, compassion, and good people close by, a parent and little one can face challenges, celebrate every small victory, and keep discovering joy in everyday moments.
Find a circle that understands—can shared experiences ease heavy moments along this journey? Absolutely. A parent connecting with families who faced similar paths often discovers comfort that words barely capture. Honest stories, practical advice, and warm encouragement can spark fresh strength during difficult days. With patience, compassion, and kind people nearby, a parent and little one can move through challenges, celebrate each small victory, and keep finding joy in everyday moments.
Stay connected with medical professionals guiding a child’s journey—could open conversation and shared planning make challenges easier to face? Absolutely. Regular updates and thoughtful coordination allow everyone involved to understand progress and adjust approaches along way, encouraging steady growth, comfort, and strong overall well-being. When family and professionals move forward as one united team, a child gains powerful encouragement and every opportunity to recover, develop, and thrive with confidence.
Author Bio:
Pamela Harris is an experienced medical writer collaborating with US Health Hub. Her focus lies in providing parents with clear, practical insights into infant wellness topics. With a talent for simplifying complex information, Pamela ensures families can easily understand important details and feel confident navigating challenges related to their little ones’ growth and well-being.