Ischemic Stroke & CT Scans: A Quick Guide
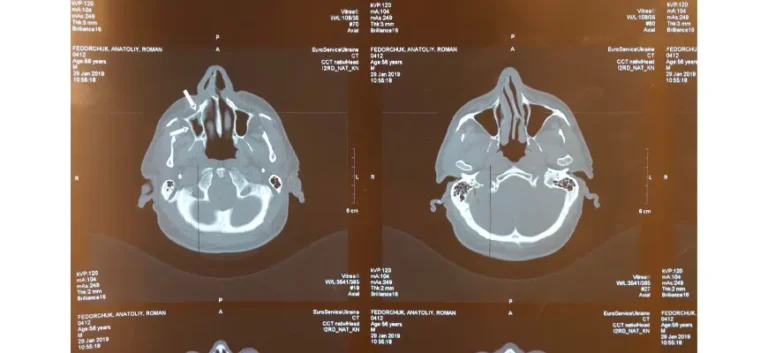
During critical medical emergencies, speed decides outcomes. Each second matters, and fast recognition plus immediate action improves results. One form appears far more often than all remaining types, reaching almost 87 percent of cases. Knowing what sets it off, how it unfolds, and how clinicians spot it so fast matters. A major tool here is a CT scan, offering rapid, detailed views inside. By looking at causes, underlying processes, and diagnostic methods, readers see why this imaging option often proves central during urgent moments.
What Is an Ischemic Stroke?
This condition happens when blood flow to a specific part of brain becomes blocked or significantly reduced. Without oxygen and essential nutrients, brain cells start dying within minutes. Picture it as a severe traffic jam in vessels supplying brain tissue. If blockage isn’t resolved quickly, damage can become permanent, causing long-term disability or even death.
Most cases result from formation of a blood clot. Clots can form directly inside brain arteries or travel from other areas, such as heart, before lodging in a vessel. Risk factors that increase chances include high blood pressure, elevated cholesterol, smoking, diabetes, and irregular heartbeat, such as atrial fibrillation.
Why Early Diagnosis Is Critical
Brain tissue is extremely sensitive. Without oxygen, cells start dying at an estimated rate of 1.9 million per minute. Every second counts when this type of emergency happens. Rapid recognition and timely intervention significantly improve chances of limiting damage and achieving better recovery.
Imaging steps forward when seconds feel heavy and uncertainty rises—why does it become first move in an urgent moment? Because speed matters, clarity matters, and confidence matters. Clinicians trust this approach since results arrive fast, access spans across facilities, and insight stays reliable for revealing conditions that disturb brain function. Could anything feel more reassuring during crisis than swift answers? Absolutely—this approach delivers direction when direction feels scarce, turning confusion into informed decisions and fear into focused resolve.
What Is a CT Scan?
An advanced X-ray–based approach captures highly refined internal visuals by rotating around a person and collecting multiple views from varied angles. Unlike basic X-ray imaging that creates a flat, single-layer picture, this approach assembles dozens or even hundreds of slices to form a complete three-dimensional view. Such layered perspective gives clearer insight into ongoing changes, especially during moments when time matters most.
When someone suddenly collapses, words tangle mid-sentence, or one side of face shifts in an unfamiliar way, this approach becomes priceless—why does urgency feel so intense? Because hidden causes can differ in life-altering ways. Could a major vessel carrying oxygen be blocked? Yes. Could bleeding follow a ruptured vessel instead? Absolutely. Outward signs may look almost identical, yet underlying events call for completely different responses to steady a life in crisis. This approach reveals truth beneath surface, guiding confident decisions when every heartbeat feels critical.
By delivering rapid, high-resolution results, this scan allows specialists to distinguish between these serious internal problems within minutes. Speed is critical, as central control center of brain—responsible for memory, movement, and vital functions—can begin sustaining permanent damage if wrong condition is treated or intervention is delayed.
This advanced X-ray approach often stands as first move in emergencies—why choose it before anything else? Because speed saves precious moments, precision sharpens understanding, and clarity replaces uncertainty. Does it truly reveal what unfolds inside head? Yes, with striking detail. Findings uncover blockages, swelling, or urgent shifts that might otherwise stay hidden. Can swift evidence shift direction in critical seconds? Absolutely. Fast insight empowers specialists to move forward with confidence, making informed decisions when every instant counts.
How does it work for diagnosis?
When sudden weakness strikes one side, speech turns slurred, or a face begins to droop, doesn’t urgency fill a room in an instant? What must happen next? Immediate response. Trained staff move fast, fully aware that even brief hesitation can cost precious time. Why start with a high-speed head check that needs no injected contrast? Because answers must come quickly in those first critical moments. This approach captures essential detail within minutes, providing clear direction while pressure rises and every decision carries real weight.
Preparation: Individuals rest on a motorized platform that moves gently into a tunnel-shaped machine resembling a large doughnut. No needles or incisions take part, keeping experience smooth and comfortable. Some may feel mild confinement, especially if sensitive to enclosed spaces; slow, steady breathing and closed eyes often ease tension.
What happens during scanning—does it feel intense or overwhelming? Not at all, it stays calm and controlled from start to finish. A machine rotates gently around head, capturing a series of X-ray images from multiple angles, and that quiet motion often feels far less intimidating than expected. Curious how long it lasts? Just a few minutes, and within that short window, clear, detailed insight into head structures comes together with impressive precision. Isn’t it reassuring to know such advanced technology works quickly while keeping experience steady and manageable? Absolutely—it brings clarity, confidence, and a sense of ease right when it matters most.
Once data gets gathered, what really brings meaning into focus? A powerful computer steps in, blending multiple angles into rich, layered views that tell a deeper story—sounds impressive, right? And what can those layered slices actually reveal? Subtle swelling, faint darkened regions, or delicate shifts in tissue that might otherwise stay hidden. Could something so slight point toward a serious concern? Absolutely, and that’s where trained eyes come in with confidence. By studying those cross-sections, specialists piece together what’s unfolding within central nervous function—so does clarity replace uncertainty in that moment? Without a doubt, because each refined layer guides understanding, turning quiet signals into clear direction when it matters most.
Interpretation: Trained specialists review visuals closely to determine if an event has occurred and identify its specific type. Insights from this review guide immediate actions, whether that involves medication, a procedure, or other measures needed to stabilize an individual.
Fast, non-invasive technology becomes a lifeline when every second carries weight—so why lean on it in moments that feel so fragile? Because clarity arrives fast and turns chaos into direction. Can clear insight drive confident, decisive steps? Without a doubt. This method brings answers within minutes, letting response teams move ahead with efficiency and steady confidence. When uncertainty starts to slow momentum, that clarity brings focus back—so does urgency shift into purpose right when it matters most? Absolutely.
What Can It Detect If Someone Has a Brain Blood Flow Problem?
In early stages, imaging may appear normal because changes within brain tissue can be very subtle. Specialists look for specific indicators, including:
Loss of Gray-White Differentiation: Have we ever noticed how certain soft tissue regions—those handling signal processing and transmission—usually show clear contrast on diagnostic images? So what happens when that contrast begins to fade or even disappear? It signals that something isn’t right. When disruption strikes within a central nervous network, distinction between those critical tissue types can blur, making separation far more difficult. Could that loss of clarity truly matter? Absolutely—it points to early trouble, turning a subtle shift into a meaningful warning that calls for careful attention and confident interpretation.
Hypodensity: Have we ever wondered what darker regions on diagnostic images might reveal? Could those shadowed areas signal something more serious beneath surface? Absolutely. Such regions often point to areas not receiving enough oxygen or essential nutrients, raising concern about what’s unfolding. Do those dimmed zones carry deeper meaning? Yes—they can indicate early tissue injury, where cells begin to struggle and function declines due to reduced circulation, turning a subtle finding into a meaningful clue that demands close attention.
Have we ever paused and wondered why delicate grooves along a central nervous network suddenly fade from view on diagnostic images? Those natural folds—called sulci—usually form crisp, recognizable patterns, so what shifts when clarity starts slipping away? Pressure builds, and nearby tissue begins to swell, pushing inward with quiet but undeniable force; as space narrows, once-sharp lines grow faint, compressed, nearly erased. Could something so subtle really carry meaning? Absolutely—it signals rising pressure that deserves immediate attention, transforming a barely noticeable detail into a powerful clue about what’s unfolding beneath surface, drawing focus, raising urgency, and guiding next steps with confidence.
Hyperdense Artery Sign: When an obstruction occurs in a main circulation pathway inside the head, it may appear as an unusually bright area on specialized internal scans. This bright signal often indicates a clot lodged within a vessel, restricting normal flow through that channel.
Have we ever noticed how faint shifts seem to whisper that something deeper is unfolding? Could a barely visible clue truly point to an urgent concern? Absolutely—it can. Even when signs look subtle or easy to overlook, experienced specialists read patterns early, stepping forward with steady confidence and clear judgment. Doesn’t that kind of early recognition make all difference? It does, turning uncertainty into direction and converting quiet warning signals into powerful opportunities for decisive, well-guided moves.
Why Is It the First Choice for Stroke Diagnosis?
Several factors make this imaging tool a top choice for diagnosing it:
Speed becomes everything when crisis strikes—can swift movement truly mean difference between loss and survival? Absolutely. One powerful advantage lies in how quickly this method finishes, often within minutes even without contrast. Does such a brief window carry real value? More than anything. Critical details reach waiting hands almost instantly, guiding teams toward clear next steps without hesitation. When each second feels amplified, does that quick clarity drive confident momentum? Without question.
Accessibility shapes outcomes in urgent moments—can advanced technology truly reach beyond major city centers? Yes, since this capability exists across facilities of all sizes, from large urban hospitals to smaller community clinics. Does such widespread presence make a real difference? Absolutely. Broad access means people in busy cities and remote regions alike can receive prompt evaluation when sudden neurological concerns arise. When distance could delay answers, availability bridges that gap—so does timely insight arrive right where and when it matters most? Without a doubt.
Precision matters most when uncertainty feels overwhelming—can very early signs always appear on this scan? Not every time. Yet when internal bleeding exists, detection remains highly reliable and clear. Why does that distinction carry such weight? Because underlying causes demand entirely different responses. One path calls for rapid intervention to stop bleeding, while another follows a separate course altogether. Accurate identification shapes every next move, turning confusion into confident, decisive action when stakes run high.
Safety often brings up an important question—does this procedure carry any real danger? Only minimal radiation exposure, and overall it remains low-risk for most individuals. In urgent moments, does waiting make sense when fast clarity can guide life-saving decisions? Not at all. Immediate understanding of what’s happening beneath the surface often outweighs concern over such small exposure levels. Can speed and precision truly justify that choice? Absolutely. Quick insight cuts through uncertainty, guides next steps, and turns critical moments into focused, confident responses when every second holds meaning.
Limitations of Brain Imaging in Diagnosis
Is this approach powerful and life-saving? Absolutely. Does it always reveal every early warning sign within first critical hours? Not always. In those opening moments, subtle shifts within brain tissue can stay quiet, almost hidden, leaving questions lingering in minds seeking clarity. Does that mean answers remain out of reach? No. Specialists press forward with confidence, turning toward advanced options like MRI to uncover what may not yet appear and to measure true extent of injury. When uncertainty shows up, does progress stop? Never. Determination fuels deeper investigation, making sure nothing important stays unseen and every crucial detail comes into view.
MRI technology can uncover subtle shifts far earlier than traditional methods—does that make it powerful? Absolutely. Yet does it always fit into urgent moments when seconds feel scarce? Not always, since process takes more time and access may be limited. So what happens when speed becomes top priority? A faster approach steps in first, delivering clear direction right away. Later, when deeper detail becomes essential, MRI joins plan—so does that added insight sharpen understanding and strengthen next decisions? Without a doubt.
What Should You Expect After Getting Your Imaging Test Back?
Once results confirm an issue, immediate action aims to reopen pathways that deliver oxygen plus nutrients to affected regions. Several advanced options exist, based on severity plus timing. One option relies on specialized medication designed to dissolve obstructions and restore circulation. When this option proves unsuitable or ineffective, clinicians may choose a minimally invasive procedure. During it, a tiny device travels through vessels to physically extract blockage. Added steps often follow to control internal pressure, steady someone involved, plus lower chances of repeat events.
Thrombolytic Therapy: Often called “clot-busting” medication, agents like alteplase (tPA) act by breaking apart obstructions that block oxygen plus nutrients from reaching vital areas of central nervous system. When given soon after symptoms begin—usually within a very narrow window—these drugs can reopen affected vessels and limit added damage to nearby tissue. Timing matters greatly, since benefit drops sharply as obstruction stays in place longer.
Ever wonder what happens when a dangerous blockage refuses to respond and every second feels critical? Mechanical thrombectomy steps in with bold precision. A skilled specialist guides a thin, flexible tube through delicate vessel pathways, navigating with focus and control—sounds intense, right? It is, and that intensity brings purpose. Once obstruction is reached, advanced tools grasp and remove it directly, restoring flow with decisive action. Why rely solely on medication when a more immediate solution exists? In moments involving severe blockage or when clot-dissolving drugs fall short, this minimally invasive approach delivers a powerful answer, offering renewed possibility when urgency demands swift intervention.
Additional Measures: Medications may be given to manage internal pressure, especially within circulatory pathways, maintaining safe balance and reducing chances of new blockages forming in critical vessels. Other interventions may be applied to reduce swelling in central control regions, helping preserve vital functions and minimize long-term damage.
How Advanced Imaging Could Change the Way We Treat Brain Emergencies
Can innovation truly transform what unfolds during a critical neurological crisis? Absolutely. Modern advances elevate technology into something far beyond earlier expectations. Perfusion methods track blood flow through brain tissue, revealing vulnerable areas before lasting damage sets in—doesn’t that shift everything? Without question. And how do hidden blockages come into clear focus? Angiography with contrast maps vessels in striking detail, exposing obstructions that call for immediate response. Isn’t precision everything in moments like this? Completely. Such advanced approaches deliver deep insight, sharpen clinical judgment, strengthen next-step strategies, and turn uncertainty into confident, life-directing decisions.
Can a moment measured in seconds decide everything? Absolutely. In urgent neurological crises, artificial intelligence steps in as a powerful ally, reading complex data almost instantly and uncovering critical shifts with striking precision. How does such speed reshape outcomes? It brings clarity when uncertainty feels overwhelming, especially in settings where expert interpretation isn’t close at hand. AI adds a vital layer of safety, catching subtle early warnings that might slip past human eyes. Is fast, confident decision-making still a distant goal? Not anymore. This evolving innovation accelerates evaluation, strengthens confidence in every next move, and turns high-pressure moments into opportunities for decisive, informed progress.
Can it detect all types of ischemic strokes?
Can this method detect every case right away? No, especially during early stages when shifts remain too subtle to appear. Does that limit value? Not at all. A non-contrast version stands strong in ruling out bleeding with solid reliability—so does that bring immediate reassurance? Absolutely. Still, can an acute event stay hidden within those first hours? Yes, it can. When deeper clarity becomes essential, options like CTA, CTP, or MRI step in—so does each one add a sharper layer of detail? Without question. Step by step, understanding grows stronger, guiding evaluation forward with confidence and clear purpose when every moment carries meaning.
How long does it take for stroke-related changes to appear on a CT scan?
Do related findings take hours to appear on a standard non-contrast approach, and does that mean nothing is happening during those first critical hours? Not at all. Early results may appear completely normal even as important shifts unfold beneath surface. Could subtle clues still emerge? Absolutely. A faint loss of gray–white distinction, slight sulcal effacement, or a hyperdense artery sign can quietly signal evolving trouble. So why look beyond basic methods in moments like this? Because advanced options like CT perfusion reveal altered blood flow much sooner, bringing hidden changes into focus and guiding smarter, more confident decisions when every moment truly counts.
Can it predict recovery outcomes?
Can a CT scan alone predict recovery with certainty? Not quite. Still, does it offer meaningful insight into how much brain damage has occurred? Absolutely. Details like size and location of an infarct, presence of swelling, and blood flow status from CT angiography or perfusion methods all add important pieces to a clearer picture—so does that information guide next steps with confidence? Without a doubt. And what truly shapes recovery beyond those findings? Factors such as age, overall condition, progress in rehabilitation, and how quickly intervention begins—does each piece matter? Completely, since together they shape the path forward with greater clarity and purpose.
Conclusion
This qualifies as a critical emergency where time decides outcomes. Advanced technology captures internal visuals with remarkable detail, allowing specialists to act fast and understand what happens inside head. Rapid response can separate a return to normal life from long-term complications. While these tools may miss some early signs, speed, broad access, and strong precision make them essential during urgent neurological events.
If warning signs appear—like sudden weakness, confusion, or trouble speaking—call 911 right away. Does every second truly matter in that moment? Absolutely, since fast response can greatly improve chances of full recovery. And how do specialists gain clarity so quickly? Advanced technology offers a quick, painless way to look inside head, delivering crucial details for timely decisions—does that level of insight change outcomes? Without a doubt, showing just how far modern medicine has come.



